Patient will present as → a 38-year-old male with a 6-month history of heartburn and regurgitation, particularly after meals, drinking coffee, and lying down. He also complains of a chronic cough, especially at night. He is overweight and has a diet high in fatty foods. On examination, he is obese, and his abdominal examination is unremarkable. A trial of a proton pump inhibitor (PPI) is initiated, and he is counseled on lifestyle modifications, including weight loss, elevation of the head of the bed, and dietary changes to avoid trigger foods. He is advised to return if symptoms persist or worsen, in which case further diagnostic evaluation, such as an upper endoscopy, may be considered.
Incompetence of the lower esophageal sphincter allows reflux of gastric contents into the esophagus, causing burning pain
- Prolonged reflux may lead to esophagitis, stricture, and rarely metaplasia or cancer
- Gastroesophageal reflux disease (GERD) is common, occurring in 10 to 20% of adults. It also occurs frequently in infants, typically beginning at birth
- Factors contributing to reflux include weight gain, fatty foods, caffeinated or carbonated beverages, alcohol, tobacco smoking, and drugs
Drugs that lower LES pressure include anticholinergics, antihistamines, tricyclic antidepressants, Ca channel blockers, progesterone, and nitrates
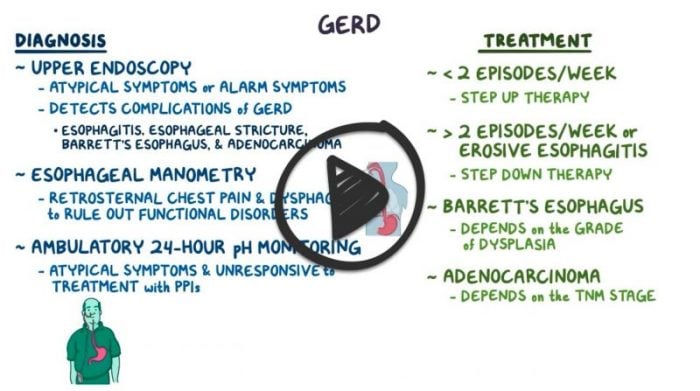
- The PH Probe study is the gold standard for diagnosis
- The upper GI study is a study of anatomy, not for reflux
- A chronic cough can be an easily overlooked symptom of GERD
- Chronic GERD may predispose to Barrett's esophagus and cancer
"Once Barrett's esophagus has been identified, screening every 3 to 5 years by upper endoscopy is recommended to look for dysplasia or adenocarcinoma. There is an 11-fold increase in esophageal adenocarcinoma in a patient with Barrett's esophagus."
Patients with foul odor of breath and increasing symptoms think Zenker's Diverticulum, which is an outpouching of the hypopharynx resulting in regurgitation of solid foods – needs surgical repair.
Patients with typical symptoms of GERD may be given a trial of PPI therapy
- Patients who do not improve or have long-standing symptoms or symptoms of complications should be studied
- Endoscopy with cytologic washings and biopsy of abnormal areas is the test of choice
- Endoscopic biopsy is the only test that consistently detects the columnar mucosal changes of Barrett's esophagus. Patients with unremarkable endoscopy findings who have typical symptoms despite treatment with proton pump inhibitors should undergo 24-hour pH testing.
- The PH Probe study is the gold standard for diagnosis
- Any patient with symptoms of GERD accompanied by dysphagia, recurrent vomiting, weight loss, hematemesis, anemia, melena, or age > 50 should undergo endoscopy as these are considered high risk for the presence of an upper gastrointestinal malignancy
Management of uncomplicated GERD consists of elevating the head of the bed about 15 cm (6 in) and avoiding eating within 2 to 3 h of bedtime, strong stimulants of acid secretion (eg, coffee, alcohol), certain drugs (eg, anticholinergics), specific foods (eg, fats, chocolate), and smoking.
- Weight loss is recommended for overweight patients and those who have gained weight recently
- Drug therapy is stepwise:
- Start with a low-dose histamine 2 receptor antagonist QD, then increase to BID if needed
- Switch to a proton pump inhibitor if symptoms persist. Start low dose and increase to standard dose if needed
- Once symptoms are controlled, treatment should be continued for at least eight weeks
| Medication | Low dose (oral) | Standard dose (oral) |
| Histamine 2 receptor antagonists | ||
| Famotidine | 10 mg BID | 20 mg BID |
| Nizatidine | 75 mg BID | 150 mg BID |
| Cimetidine | 200 mg BID | 400 mg BID |
| Proton pump inhibitors (PPIs) | ||
| Omeprazole | 10 mg QD | 20 mg QD |
| Lansoprazole | 15 mg QD | 30 mg QD |
| Esomeprazole | 10 mg QD | 20 mg QD |
| Pantoprazole | 20 mg QD | 40 mg QD |
| Dexlansoprazole | Not available | 30 mg QD |
| Rabeprazole | 10 mg QD | 20 mg QD |
 Osmosis Osmosis |
|
 |
GERD is the reflux of gastric contents into the esophagus, which is characterized by inflammatory symptoms resulting from the irritating effects of gastric or duodenal contents on the esophageal mucosa. Patients who are obese are at increased risk for the disease due to increased intra-abdominal pressure, which allows the reflux (backward flow) of stomach contents into the esophagus.
Play Video + QuizQuestion 1 |
Eating smaller meals at a time Hint: Eating smaller meals at a time reduces symptoms of GERD. | |
Elimination of acidic foods Hint: Elimination of acidic foods reduces symptoms of GERD. | |
Weight loss; stop smoking and alcohol ingestion Hint: Weight loss; stop smoking and alcohol ingestion reduces symptoms of GERD. | |
Lying down within 3 hours after meal |
Question 2 |
Proton pump inhibitors (PPI) | |
The dopamine antagonist prokinetic agents Hint: The dopamine antagonist prokinetic agents are not as effective as PPIs. | |
H2-receptor antagonists Hint: H2-receptor antagonists are not as effective as PPIs. | |
Alginate-containing antacids Hint: Alginate-containing antacids are not as effective as PPIs. |
Question 3 |
Barrett’s esophagus | |
Zenker’s diverticulum | |
Gastritis | |
Diffuse esophageal spasm |
Question 4 |
Hiatal hernia contributes to the development of GERD. | |
Excessive reflux is defined as a pH <4 for >4% of the time | |
In most patients with GERD, baseline LES pressures are normal (10–35 mm Hg). | |
Endoscopy is indicated in all cases of GERD. |
Question 5 |
True | |
False |
Question 6 |
Zenker's diverticulum | |
Peptic Ulcer Disease | |
Achalasia | |
Gastric Cancer | |
Pyloric stenosis |
|
List |
References: Merck Manual · UpToDate




