| Autoimmune Hemolytic anemia | Patient will present as → a A 30-year-old woman presents with fatigue, pallor, and jaundice. She reports experiencing dark urine and a recent unexplained weight loss. Her medical history includes systemic lupus erythematosus, treated with hydroxychloroquine. Physical examination reveals splenomegaly and mild tachycardia. Laboratory tests show anemia with elevated reticulocyte count, indirect bilirubin, and lactate dehydrogenase. Direct Coombs test is positive, confirming a diagnosis of autoimmune hemolytic anemia. She is started on prednisone, with a significant improvement in her hemoglobin levels and symptoms over the following weeks. Increased destruction of erythrocytes due to the presence of anti-erythrocyte autoantibodies (AEA) ↓ Hemoglobin/hematocrit, ↑ Retic, ↑ LDH, ↓ Haptoglobin, ↑ Bilirubin (indirect), and + Direct Coombs Test Some people have no symptoms, and other people are tired, short of breath, and pale
Treated with corticosteroids
Common in all hemolytic anemias: • Elevated reticulocyte count, LDH • Decreased haptoglobin and hemoglobin/ hematocrit
Common to autoimmune anemia:
|
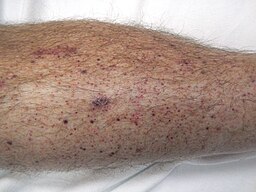
| Immune Thrombocytopenic Purpura (ITP) | Patient will present as → a 39-year-old female presents with concerns about sudden onset nosebleeds and a rash on her legs. She recalls a mild viral illness about three weeks ago. She is otherwise healthy and takes no regular medications. On examination, her oral mucosa is noted to have spontaneous bleeding, and her legs reveal widespread petechiae and a few larger purpura. Her abdomen is soft and nontender, and there is no palpable splenomegaly. Laboratory tests show a platelet count of 30,000/μL (normal 150,000 – 400,000/μL). The peripheral blood smear indicates a decreased number of platelets without clumping. The rest of her complete blood count, including white blood cell count and hemoglobin, is within the normal range. She is started on corticosteroids. ITP results from autoimmune antibody formation against host platelets CBC normal except ↓ low platelets (<20,000) and + Direct Coombs Test In children, it may follow a viral infection. In adults, it may be chronic
Symptoms may include easy bruising, bleeding, and petechiae (pinpoint-sized reddish-purple spots) on the lower legs Treated with corticosteroids
|
| Pernicious anemia | Pernicious anemia is an autoimmune disorder caused by an autoantibody formation against intrinsic factor, a glycoprotein essential for vitamin B12 absorption
Megaloblastic anemia (↑ MCV > 100), hypersegmented Neutrophils, + schilling test*, ↓ intrinsic factor, and anti-intrinsic factor antibodies (increased)
TX: Parenteral therapy is preferred—cyanocobalamin (vitamin B12) IM once per month Schilling test—historically used to determine if B12 deficiency is due to pernicious anemia. Not routinely used now.
|